
Health equity refers to the idea that everyone should have the same opportunity to be healthy, regardless of their social or economic background. The problem with health equity is that certain groups of people may face barriers to accessing healthcare and other factors that contribute to good health. This can lead to health disparities, where some groups have higher rates of illness and shorter life expectancies than others.
Health inequities can be caused by various factors, such as poverty, discrimination, and the unequal distribution of resources. It is important to address these issues to ensure that everyone has an equal opportunity to be healthy and live a full, productive life.
One of the most important issues in the current healthcare system is the widening gap between those who can afford quality healthcare and those who cannot. As a result, there is a lot of talk about digital health solutions as a way to close this gap.
However, this is just a wish, not a reality. From our experiences in building digital health solutions both in developed and underdeveloped countries, we discovered that digital health solutions are not inclusive enough.
While I was writing this article, the results of the WHO Europe study came out, which showed that we were right.
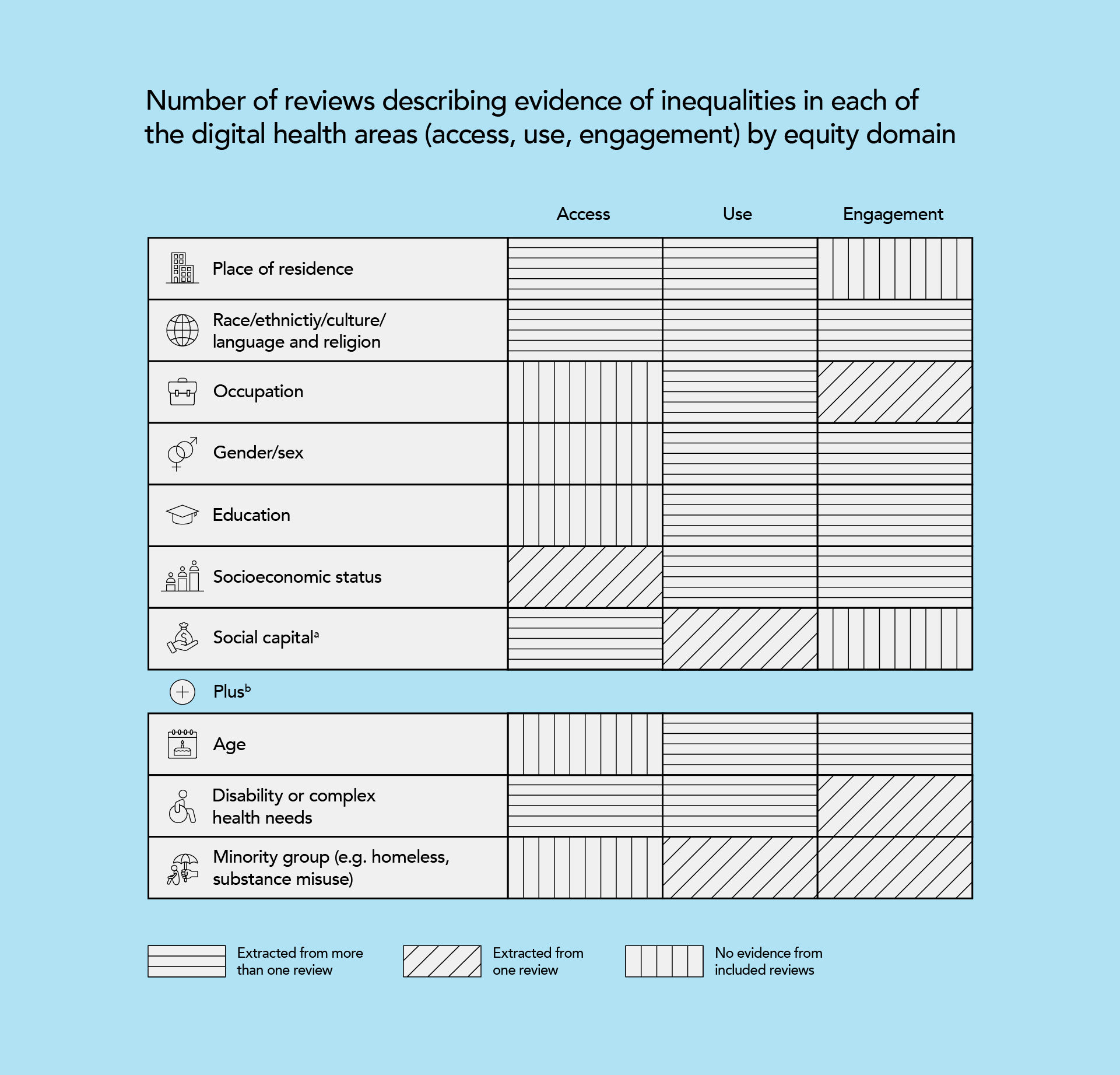
Source: Equity within digital health technology within the WHO European Region: a scoping review: 2022.
There are several challenges to achieving “digital health equity,” which refers to the equal access and use of digital health technologies and services by all individuals. Some of these challenges include:
Socio-economic status
Some people may not have the digital literacy skills they need to use digital health services and technologies for various reasons:
- Access to technology and affordability: digital health technologies and services can be expensive, which may be a barrier for some individuals.
- Internet connection: Even if a person has the right tools, they might not have a reliable way to connect to the internet, which is needed to use digital health services.
Race/ethnicity/culture/language
Race, ethnicity, culture, and language can all have an impact on a person’s ability to learn and use digital technologies.
For example, language barriers can make it difficult for some individuals to access and use digital resources, as much of the content and interfaces for these technologies are in English or other widely spoken languages. This can be especially challenging for individuals who are not fluent in these languages or who come from cultures where the use of digital technologies is not as prevalent.
Cultural differences can also play a role in an individual’s willingness to adopt and use digital technologies. For example, some cultures may place more value on face-to-face communication and be less likely to use digital forms of communication.
Additionally, there may be racial or ethnic disparities in access to digital technologies. For example, studies have shown that African Americans and Hispanics are less likely to have access to the internet and other digital technologies compared to their white counterparts.
Age, disability, or complex needs
Age, disability, and having a lot of different needs can all make it harder for a person to learn and use digital technologies.
Older adults may be less familiar or comfortable with using digital technologies and may need additional support and resources to learn how to use them.
Individuals with disabilities may face additional challenges in using digital technologies, as many of these technologies are not designed with accessibility in mind. For example, someone who is blind or has “just” dyslexia or color blindness may not be able to use a device with a visual interface, and someone who is deaf may not be able to use a device that relies on sound. As stroke is among the leading causes of disability in the world, a lot of people must deal with aphasia, which might severely impact their ability to interact with digital tools.
People with complex needs (e.g., the homeless, substance addicts, intellectual disorders, war veterans, etc.) may also find it hard to use digital technologies because they might not be able to adapt to their needs or abilities.
Ethical concerns
There are also ethical concerns about digital health equity, such as the possibility of biased algorithms or the unequal distribution of benefits and harms.

The aforementioned challenges are vectors of the digital health inequity force, which is getting its own name — the digital health divide.
The digital health divide will undoubtedly result in disparities in healthcare access and outcomes if not addressed upfront. Accessibility is a key quality, and as with all key qualities, it is extremely hard and costly to retrofit. Therefore, closing the digital health equity gap is only possible by being aware of it, being proactive, and engaging with all relevant stakeholders from day zero. Otherwise, the new shiny digital health solution would just widen the health equity gap, as those who are unable to use digital health technologies and services may miss out on critical healthcare information and services.

Let me also shed some light on another area of digital health equity that is often overlooked: healthcare professionals. We are all getting older, and consequently, our health is not getting better. When we think of healthcare professionals and their interactions with digital health solutions, we often imagine the ideal user: young, digitally literate, and eager to try out new toys like IoT, Metaverse, and AI/ML.
However, there is significant friction in digital health adoption among healthcare professionals. To illustrate the increasing gap, I will give you this statistic about eHealth literacy among medical students, performed by the WHO: According to the WHO, less than 25% of health sciences students receive preservice training in eHealth, and more than 75% of health professionals receive in-service training in eHealth .
We should not neglect this reality, as if we do nothing, we might get a very vocal and powerful group of key users preventing success. Having healthcare professionals on the project team is essential for establishing trust and reducing fear of novelty among this critical group of users.

For sure, many approaches can lead to successful inclusion of everyone in the health equation. Our driving principles for delivering inclusive solutions are:
- Understand and be holistic
- Treat equity as quality
- Improve
Understand and be holistic
If you don’t see the problem, you cannot fix it! As a result, at HTEC, everything begins with empathy and a thorough understanding of the actual needs and values hidden behind frequently exaggerated and superficial functional requirements.
To be holistic, we must consider not only potential users but also their ecosystems, secondary influencing users, knowledge sources in their human circles, all motivating and influencing factors, the target users’ trusted people and agents, and finally, the negative factors that may jeopardize our efforts.
Therefore, it is critical to assemble a diverse and interdisciplinary team, particularly in the healthcare and life science domains. Depending on the project and how the client’s team is set up, we have the following experts on the team:
- Healthcare professionals, such as doctors, nurses, specialized nurses, occupational therapists, psychologists, etc., who represent the professional side
- Human factors engineering (HFE) tries to understand and model patient and healthcare professional interaction with the system using modern human-centric design techniques and product design
- Research specialists who are focused on understanding user needs and providing a solution which will cover all UI/UX aspects thus making easy-to-use solutions that will solve problems
- Quality and compliance expert who strategizes and oversees alignment with required regulations and guidelines
- A risk management expert can help figure out if the benefits of using the solution outweigh the risks that might come with it
- A person responsible for patient and public involvement activities while ensuring that the views and experiences of patients and the public are considered in the planning, design, delivery, and stage evaluations. This involves working with patients and the public to identify their needs and preferences, create strategies and plans for successful implementation, and present their interests to us, our clients, healthcare organizations, and researchers.
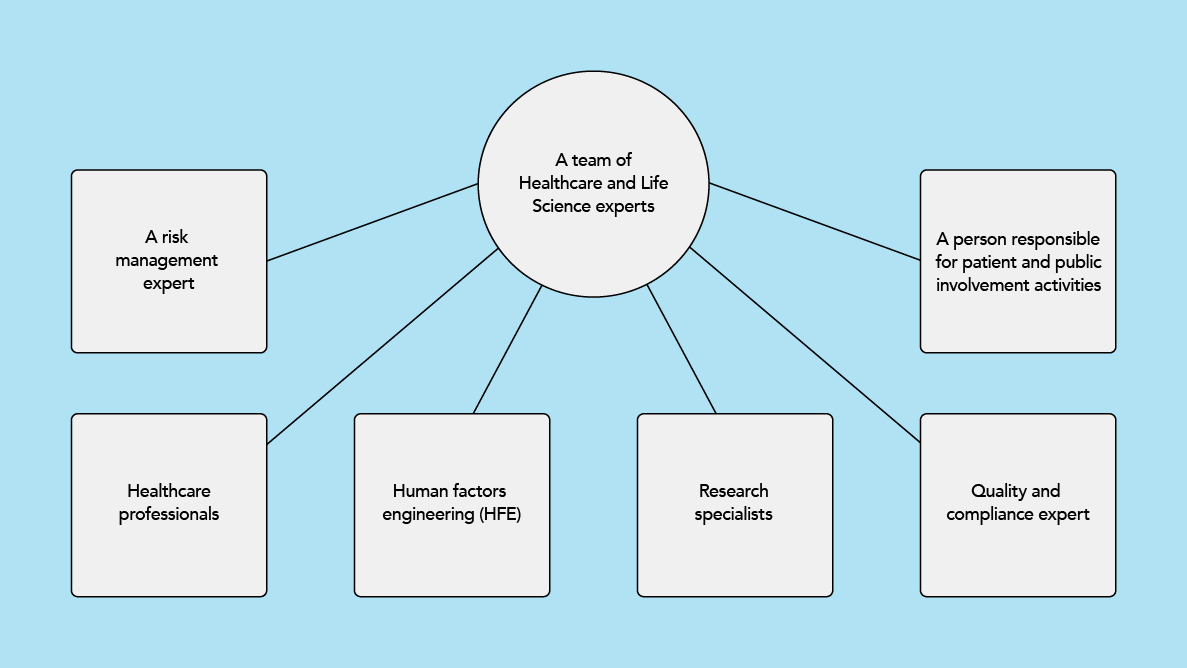
Over the past few years, our management team has considered the importance of having diverse social capital, cultures, and demography along with the best talent. The set strategy delivered. As a result, we can quickly assemble competent, emphatic, and driven teams.
The team starts their journey by considering the various ways in which people with different abilities or disabilities, beliefs or cultural backgrounds, and social and economic status might interact with the technology we design and identifying any barriers or challenges that they might face along the way.
The 360-degree assessment does include not only patients and healthcare professionals but also other parties coming from the interested public and NGOs.
Once the problem areas are identified, and the solutions to tackle them are aligned, HFE and UX experts design verification and validation approaches. But what do these experts essentially do? Well, typically their core activities include:
- Performing desk research to gain a deeper understanding of the users’ context, pains, needs and gains. Consider all the factors that might impact user inclusivity and the overall experience with the solution.
- Through understanding the user’s context, it is possible for them to effectively map the ecosystem and identify all the relevant stakeholders that are essential for creating an inclusive solution.
- Creating user personas, which are fictional characterizations of the potential users’ essential characteristics, which include their demographics, language proficiency, health profile, health needs, knowledge, attitudes, practices, and motivations.
- Drawing a user journey map of the users’ end-to-end activities and processes to display a full range of steps and potential routes to arrive at a specific result. The main user pain points, obstacles, and opportunities can be highlighted using a user journey map. It provides information not only on what digital solution will be developed but also on related topics, like the user onboarding procedure. Although it is frequently disregarded, the onboarding process is one of the most significant obstacles to adoption (some methods for creating an efficient and inclusive onboarding procedure will be discussed later in the text).
- Finding any potentially harmful interactions with the solution, analyzing them together with risk management experts and potential end users, and taking steps to prevent them.
- Designing and validating user scenarios for crucial points in the user’s journey that describe particular user’s needs in simple, action-oriented “stories.” Simply put, user stories explain what users must do and why. To ensure the stories accurately written by solution development team reflect reality, it is crucial to validate them through user research.
- Designing low-level and later more detailed prototypes of the digital solution. While paper prototypes and low-level wireframes may not have fine-grained details, they have the advantage of being an affordable and proven method for quickly testing high-level concepts with users without distracting them with aesthetic details. These low-fidelity artefacts enable us to receive early feedback on the degree to which the overall user interface, including its language and navigational flow, is consistent with the users’ mental models, needs, and context. The artefacts, at the very least, facilitate discussions with users to clarify the problems at hand and give us a chance to see if we are going in the right direction without spending money on something that will not be used.
- Testing a critical component of the design process. Once a prototype is developed, all assumptions are again tested with the diverse potential end-user cohort to prove we will deliver on the digital health inclusion promise.
- Iterating. Prototypes are created based on preliminary understandings and research, and users are asked to provide feedback. The design is adjusted as needed, and the process is repeated until the solution meets the user’s requirements. This incremental approach is critical for maintaining a short design-test-adjust validation loop.
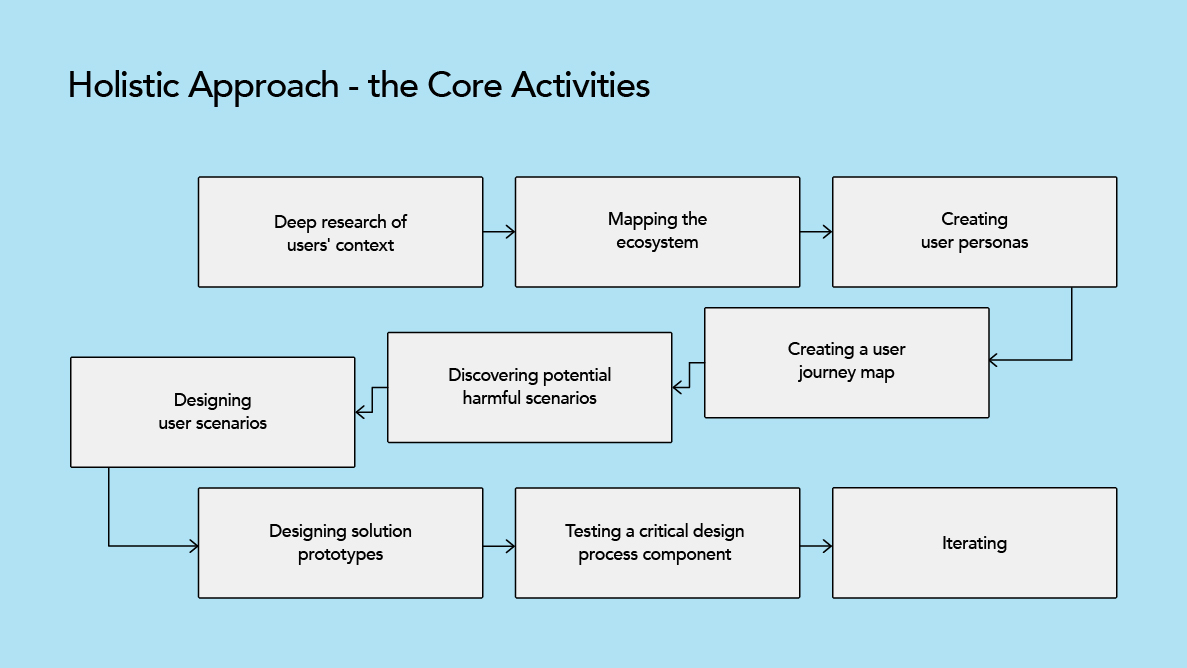
Besides having a dedicated team of experts who will discover problems, offer solutions and design verification and validation approaches, there are a few more important things to keep in mind when implementing a holistic approach to successful inclusion of everyone in the health equation. These include:
– The onboarding processes
– The importance of language proficiency
– Leveraging key communication channels
Onboarding process: well begun is half done
An accessible and fluent onboarding process is important for an inclusive web application because it helps to ensure that all users, regardless of their abilities or disabilities, can understand and use the application effectively. At HTEC, we believe that the following are the key qualities of an inclusive onboarding process:
- Easy to use and navigate: The onboarding process should be clear and easy to follow so that users of all skill levels can understand and complete it.
- Compatible with assistive technologies: The process should work with assistive technologies like screen readers so that people with disabilities can access and use the digital solution.
- Adaptive to different devices and browsers: The process should be adaptable to different devices and browsers so that users can complete the onboarding process regardless of the device or browser they are using. Support different internet bandwidths to reach as many users as possible.
- Translatable: The process should be able to be translated into different languages to ensure that users who speak different languages can understand and complete the onboarding process.
- Informative, yet easy to understand: The process should use clear and concise language and instructions to ensure that users can easily understand what is required of them.
- Supportive: The process should offer help and support to users who are having trouble getting started, such as through a help center or live chat.
- Accessible: The process should be accessible to users with disabilities, including those with visual, auditory, motor, and cognitive impairments. This could include using different formats, like audio or video, and giving instructions and guidance that are clear and easy to follow.
- With Plan B at hand: When users, for whatever reason, are unable to do it themselves, there must be a proxy option to deliver care to the ones in need.
An accessible onboarding process can also help to improve the overall user experience by making it easier for users to get started with the application and understand its features and functionality. This can help increase user engagement and satisfaction and contribute to the success of the application.

The importance of language proficiency
While designing user personas, mapping the user journeys, creating usage scenarios, and validating the assumptions with a prototype, we should give extra focus on the language proficiency of all potential users. Language understanding, both written and spoken, is one of the greatest inhibitors to the delivery of optimal healthcare. It can affect health equity in several ways.
For example, if a person is not proficient in the dominant language spoken in their community, they may have difficulty accessing healthcare services. They may not be able to understand the information provided by healthcare providers or be unable to communicate their symptoms or concerns effectively. This can lead to inadequate or delayed healthcare, which can have negative consequences for their health, represent a major financial burden to payers, and overload the already stretched healthcare system.
In addition, language barriers can also affect a person’s ability to advocate for their own health and make informed healthcare decisions. For example, they may not be able to understand the risks and benefits of different treatment options fully, or they may be unable to communicate their preferences to their healthcare providers.
There are several ways that digital health solutions can address language proficiency to improve health equity. At HTEC we leverage the multidisciplinary project team’s ability to engage with end users and the interested public to embed the following into the solution from day zero:
- Offer language translation options to make it easier for users who do not speak the dominant language to access and understand information. We should include options for open-source translations and deploy them on the live system.
- Provide language-specific content to ensure that information is accurately and effectively conveyed to users who speak different languages. For example, language specific media including video or audio content or captions on the page.
- Offer language-specific support, like chat or email support, to help users who don’t speak the dominant language communicate with healthcare providers or support staff.
- Use plain language so it is easier for users with a wide range of language proficiency levels to understand the message.
Leveraging key communication channels
Reach as many as possible.
This is a hard nut to crack, especially in underdeveloped countries and regions. The road to solving difficult problems is not always easy, but it is always worth it in the end. There is not much we can do when we have to deal with infrastructure problems because technology is not equally available everywhere. But we should develop strategies to find new ways to achieve equal healthcare.
There are a few strategies that could be used to reach everyone, everywhere, with digital health solutions, including:
Partnering with local organizations and community leaders as well as international organizations and development funds. Digital health solutions can be used and promoted more effectively in rural areas if local organizations and community leaders work with them. Therefore, the project team needs to be made up of people from different fields and have a person whose job it is to make sure patients and the public are involved.
Make use of existing infrastructure and digital solutions: In rural areas, it may be more cost-effective to use existing infrastructure, such as schools or community centers, to provide internet access and digital health services. There are many reasons why it is important to use existing technologies and solutions:
- Cost-effectiveness: Reusing existing technologies and solutions can be more cost-effective than building new ones from scratch. This is especially important when resources are limited in low-income or underserved communities.
- Time efficiency: Reusing existing technologies and solutions can save time and allow teams to focus on other aspects of the project rather than having to start from scratch.
- Scalability: Using existing technologies and solutions can help make the digital health solution more scalable because it can be built on and changed to meet the needs of different communities or populations.
- Sustainability: Using already-existing technologies and solutions can help make sure that the digital health solution will be around for a long time since it won’t have to be built from scratch every time.
Use multiple communication channels. Do you recall how Twitter overcame censorship during the Arab Spring to deliver on the free speech promise? Reaching rural populations may require using a variety of communication channels, such as SMS, radio, and community meetings, in addition to more traditional channels like the internet.
Design low-cost, low-tech solutions. In areas with limited infrastructure, it may be necessary to design and build low-cost, low-tech solutions that can still give users valuable health information and services.
Train and empower local healthcare providers. Providing training and resources to local healthcare providers can help to ensure that they are able to use and promote digital health solutions in their communities effectively. The only way to be able to grow and reach more people over time is to use the knowledge of local healthcare professionals.
Use interoperability standards. Interoperability standards allow healthcare data to be shared between different systems and platforms. This can improve the accuracy and completeness of healthcare records and help healthcare providers in the field make better decisions.
Treat equity as quality
Once all potential inequity contributing factors were identified and mitigated in the previous “stage”, now is the time to transform the unmet needs, innovative approaches, user journeys, and prototypes into a set of SMART goals.
These goals are then refined and augmented with quality and compliance requirements by an interdisciplinary project team, together with the users and client representatives. Our compliance experts review the existing regulatory framework, including country/ region-specific digital solutions accessibility policies (like the UK NHS Accessible information standard or EU Accessibility Act or US Law). If there are no such regulations or guidelines, we insist on delivering at least the AA accessibility level according to the WCAG 2.1 standard.
During the planning, designing, and development of the product’s iterations, we follow the following principles:
- Treat all requirements equally. Giving equal importance and consideration to all types of requirements during the design and development process. Functional requirements are the specific features and capabilities a solution should have, such as the ability to perform a certain task or process data in a certain way. Non-functional requirements, on the other hand, are the quality or performance characteristics of the solution, such as usability, accessibility, reliability, security, performance, etc. By treating both types of requirements equally, designers and developers ensure that the software application meets all the necessary requirements to function correctly, be inclusive, and perform optimally. This helps to ensure that the software is fit for purpose and meets the needs of all users.
- Carry out user testing and catalogue new insights. User testing helps developers identify and fix any issues with accessibility, usability, or misunderstood features in the application before it is released to the public, which prevents any potential trust issues when going live. By learning from user testing, developers can continuously improve the design and functionality of the application to meet the needs of the users better. This helps to ensure that the application remains usable and accessible over time, even as user needs and technologies change.
Improve
There is no such thing as a perfect first release. It is important not to settle with the first wins but to continue amplifying the feedback loop, gaining a better understanding of the whole picture, usage patterns, issues, and possible adverse events.
Integrating newly identified facts into the planning, designing, and verifying of new improvements is vital for ensuring safety, medical benefits, business value, high quality, compliance, and user satisfaction. To ensure success, you need a process for continuous improvement that lets you respond quickly and make small changes to the design.
Keeping engaged with the users after the solution is used is invaluable to be able to keep the solution as relevant as possible for a prolonged period.
Bridging the digital health divide
Studies suggest that the anticipated benefits to health and care systems include delivering more efficient and effective care closer to patients and targeting scarce resources better using precision medicine, big data, and artificial intelligence. Other potential benefits include reducing unnecessary hospital readmissions and improving patient outcomes. Individuals are expected to reap benefits such as quicker access to information and more personalized care, as well as increased control over and empowerment in matters pertaining to their own health.
What were the motivations behind digital health? Well, this is a long list, but it can be summarized with the following promises:
- Improved health outcomes with the optimized cost of care
- Improved access to healthcare — Make it easier for people to access healthcare services, particularly in remote or underserved areas
- Increased efficiency — Help streamline and automate different parts of healthcare, which makes them more efficient and saves money
- Digital health technologies can make it easier for patients to be more involved in their own health care, such as through telemedicine and personal health tracking devices
- Better management of data — Help collect, store, and analyze a lot of data, which can help people make better decisions and better manage the health of the whole population
- Better communication — Help healthcare providers talk to each other and work together better, which helps deliver care more smoothly and work better.
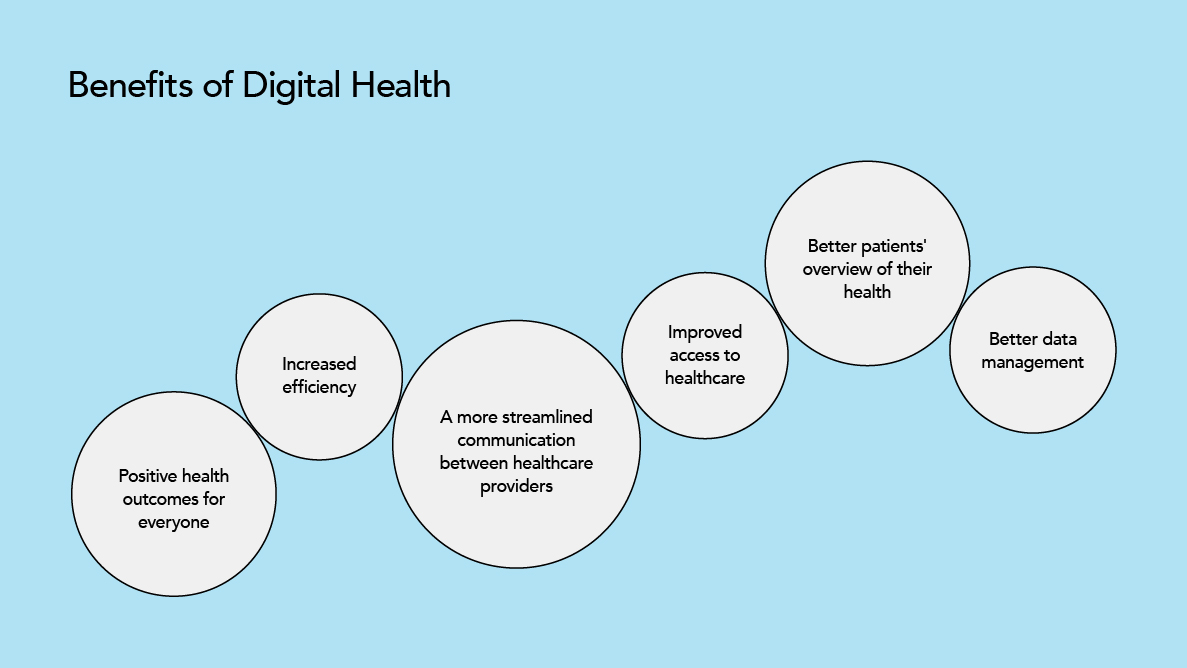
Did we deliver? Yes, and no. We are still learning and getting better. For sure, the digital health divide is a reality, just as other digital divides are. As digital healthcare is a relatively “young” industry, we are still in time to prevent the widening of this gap and use the technology in a way that will enable the closing of the general healthcare equity gap.
HTEC is well-equipped, prepared, and aware of the challenges ahead in the healthcare and life science industry. In HTEC, patients and healthcare professionals have found a strong ally in advocating access to quality healthcare for everyone, everywhere. We are on a mission to delight, not just deliver.






